INTRAPEC Technique Controls Pectoralis Spasm and Pain for Subpectoral Breast Implantation - A Retrospective Study
Published: Plastic and Reconstructive Surgery - Global Open
Of the 17 study participants, 13 (76.4%) reported spasm scores less than 3 for the entire 2-day study period and, at most time points, patients reported a median score for pain of 2, with IQRs ranging from 1 to 7.
Reliable needle visualization during ultrasound guided regional and vascular procedures. A simple solution to steep angle echogenicity loss with any ultrasound system, based on target depth
Ultrasound-guided regional anesthesia is now recognized as the evolving alternative to standard landmark-based techniques for nerve blockade and vascular access. e limitations of this technique begin to be recognized, however, as needle angles increase beyond 30 degrees, as commonly used for deep injections. This limitation remains di cult to overcome, especially for novice users.
Accuracy in evaluating gastric ultrasound images before and after brief training
The objective assessment of gastric volume by ultra- sound imaging can contribute valuable data for pre- operative evaluation. Anesthesia providers can use the information to modify the plan of care as needed to reduce the risk for anesthesia-related pulmonary aspiration in surgical patients. We presented a 45-minute instructional activity to nurse anesthesia students (N=110) who had no prior experience with interpreting gastric ultrasound imaging.
Ultrasound guidance in anesthesia
Sonography ultrasound addresses a variety of concerns, such as patient safety and comfort, cost-effectiveness, time to complete a procedure, and success rates associated with invasive anesthesia procedures. Ultrasound guidance is commonly being used for the placement of nerve blocks, placement of peripheral and central lines, and arterial catheterization.
Detection of pneumothorax with ultrasound
Diagnosis of a pneumothorax in the perioperative area can be difficult. Traditional gold-standard modalities may not be available or feasible to institute. Ultrasound guidance allows the anesthesia provider a method of quickly ruling out this potentially life-threatening complication. In this article we detail the use of sonography for fast and accurate diagnosis of pneumothorax.
Ultrasound-guided placement of combined superficial cervical plexus and selective C5 nerve root catheters: a novel approach to treating distal clavicle surgical pain
Treating the pain that patients experience from repair of distal clavicle fracture can be a challenge for the anesthesia provider, possibly because of the dual innervation in this region. Dual innervations of the distal clavicular region also make selecting the correct regional block difficult. This article describes the first successful use of 2 separate ultrasound-guided perineural catheters placed for the purpose of treating distal clavicle pain and maintaining the analgesia.
The Evolution of the Adductor Canal Block: The Emerging Technique for Motor-Sparing Analgesia to the Knee
This article summarizes current relevant data regarding the adductor canal block. It provides readers with background information of this emerging technique, including history, review of literature, relevant anatomy, and the technique itself.
Use of clevidipine for intraoperative hypertension caused by an undiagnosed pheochromocytoma: a case report
The acute intraoperative hypertension and tachycardia caused by an undiagnosed pheochromocytoma is a rare event for the anesthesia provider. If treatment is not prompt and successful, permanent and possibly lethal complications can ensue. This article reports what the author believes to be the first case study in which clevidipine (Cleviprex) was successfully used to treat a suspected, and later diagnosed, pheochromocytoma.
Letter to the Editor- response...
I have read the letter by Mr. Smith, and congratulate him on a well articulated work. He raises interesting points from the article published by the AANA Journal in February 2013 regarding the novel technique of an ultrasound guided combination of C-5 selective root and cervical plexus catheter placement for the treatment of distal clavicle surgical pain (1). If you will permit me, I would like to address some of his concerns.
Ultrasound guided INTRAPEC injection: A simple solution for surgical field improvement during electrocautery, implantation and expansion for breast reconstruction.
Regional anesthetic techniques for plastic surgery present a particular set of challenges for the anesthesia provider. Two recognized issues are the complex, wide and sometimes not well described pain generators from extensive areas involved with plastics procedures, and the risk of LAST (local anesthetic systemic toxicity).
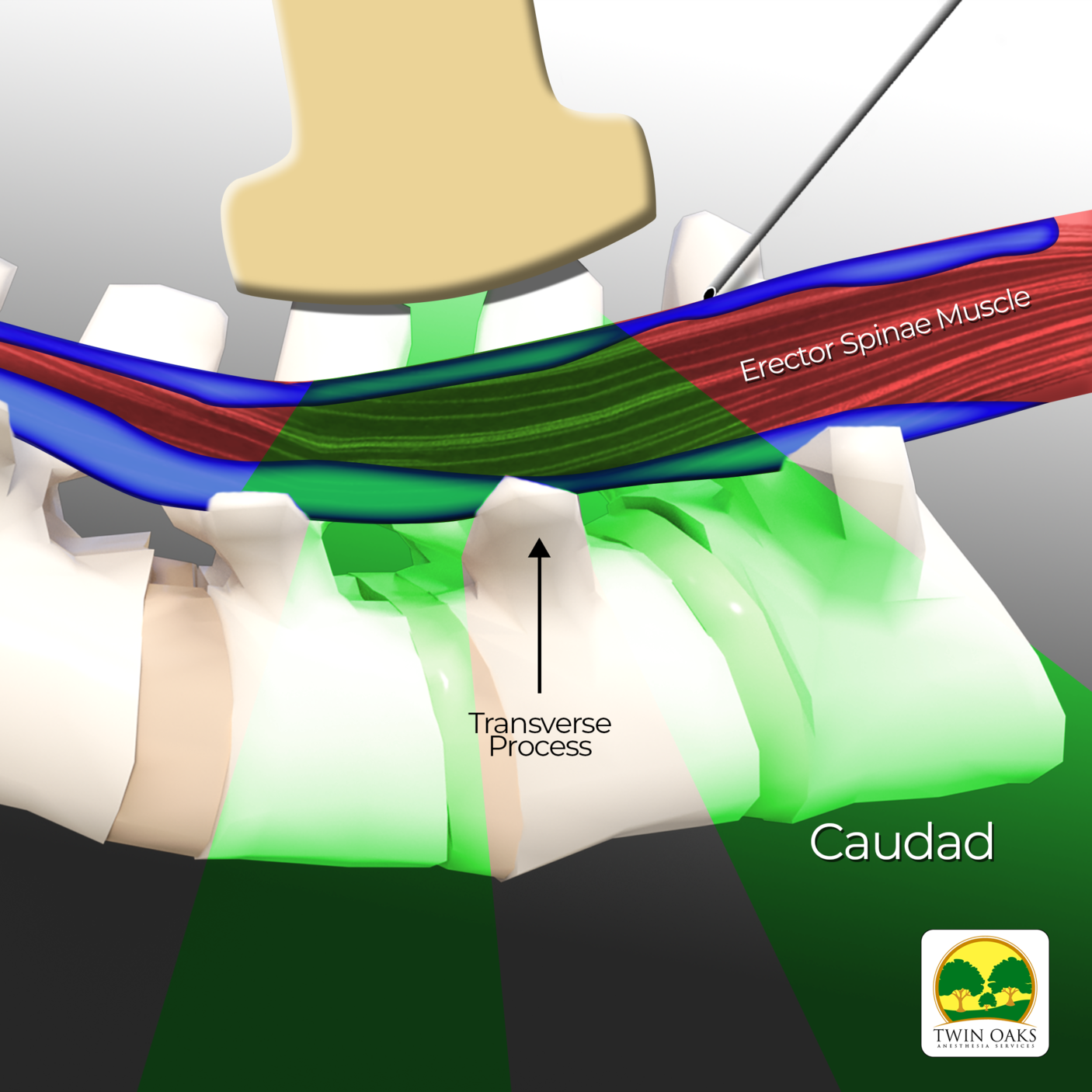
Modified dual-injection lumbar erector spine plane (ESP) block for opioid-free anesthesia in multi-level lumbar laminectomy
The erector spinae plane (ESP) block has been used to provide opioid-sparing analgesia in lumbar spine surgery, with the dorsal rami of spinal nerves as the primary target of action. 1 However the ensuing nerve blockade with fascial plane blocks may not always be dense or complete, as evidenced by inconsistent loss of cutaneous sensation to cold or pinprick testing.2
Discovery of a Pectoral Nerve Neuroma by Procedural Ultrasound Before Breast Reconstruction Surgery: Case Report
Chronic pain from breast surgery seems to be commensurate with and increase the number of breast surgeries. Many
improvements have been made in both surgery and anesthesia techniques. These novel techniques have shown promising
results in decreasing postoperative pain and opioid use, along with the cascade of undesirable side effects, and even cancer
recurrence.
INTRAPEC Injection with Liposomal Bupivacaine Mixed with Bupivacaine Can Prolong Postoperative Control of Pectoral Spasm After Subpectoral Breast Implantation: Case Report
This case study reports the use of a liposomal bupivacaine and bupivacaine (Marcaine) mixture as the agent for INTRAPEC injection, leading to prevention of intraoperative and postoperative pectoralis muscle spasm from subpectoral breast reconstruction. Liposomal bupivacaine is a high-concentration slow release formulation of bupivacaine encapsulated in liposome known as DepoFoam.
PENG Block
The quest for a single shot regional technique that provides adequate analgesia for hip fracture, and subsequent surgery has captivated a generation of new frontier anesthesia providers for well over a decade. While the introduction of fascia iliaca block brought new life in to this seemingly impossible task, it has certain clinical facets that have made it considerably less desirable to routinely deploy.